Blog Post by Erika Lassig
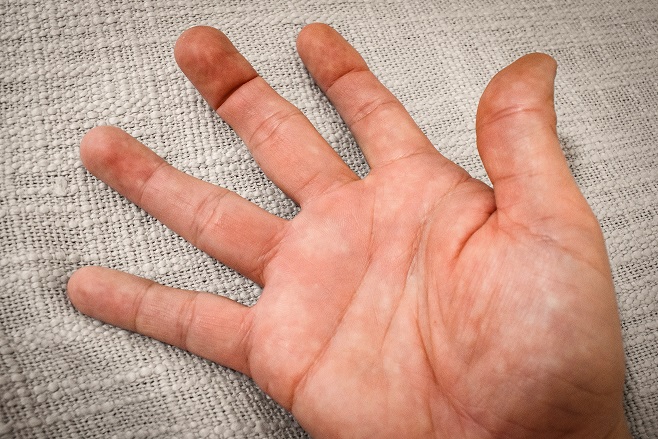
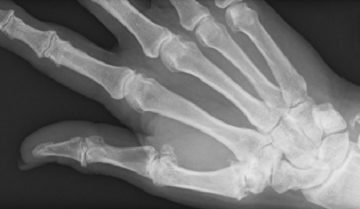
The most common thumb joint injury is called Skier’s Thumb or Gamekeeper’s Thumb. It occurs when the thumb is stretched too far away from the hand accidentally during a fall or playing sport. One of the supporting thumb ligaments is sprained or pulled off the bone with or without a small piece of bone attached. The thumb is usually swollen and painful to move, particularly when stretching it out or pinching and gripping. Often there is no sign of injury on x-ray, however there will be pain and sometimes instability of the joint indicating a ligament injury.
The ligament in question is called the Ulna Collateral Ligament (UCL) of the thumb metacarpophalangeal (MCP) joint. The good news is that most thumb UCL injuries recover well with therapy! There is only a small number that require surgery and in these cases it is because the ligament gets caught in some other soft tissue structures and cannot mend to the bone. This is called a Steiner Lesion and can be diagnosed on MRI if instability in the joint continues after casting or splinting treatment.
If you have a suspected Skier’s thumb injury, you will need to protect the injured ligament for 4-6 weeks in a splint or cast. A plaster cast is a cheap and effective way to rest injured joints, however if both the wrist and thumb are immobilised, then stiffness nearly always results. A hand therapist can provide you with a custom-made splint or orthosis, that only limits a small amount of thumb movement to protect the ligament but allows you to continue using your hand for many things. The splint is also removeable, allowing you to wash your hand and do some gentle movement exercises aimed at preventing stiffness.
Ligaments have poor blood supply and as a result take along time to heal. A hand therapist will be gradually increasing exercises, introducing strengthening at the appropriate time and giving advice regarding return to more demanding activities such as sports.
If you think you have a Skier’s Thumb injury, book an appointment with us today so that you can get back to what you love.